What Is Plantar Fasciitis?
Plantar Fasciitis seems to be quite a common complaint of many of my clients at the moment so I thought I would talk about it today.
Plantar Fasciitis is very common. Approximately 1 in 10 people will develop plantar fasciitis at some point in their lives. It is most common in people between the ages of 40 to 60. However, it can occur at any age. It is twice as common in women as it is in men. It is also common in athletes.
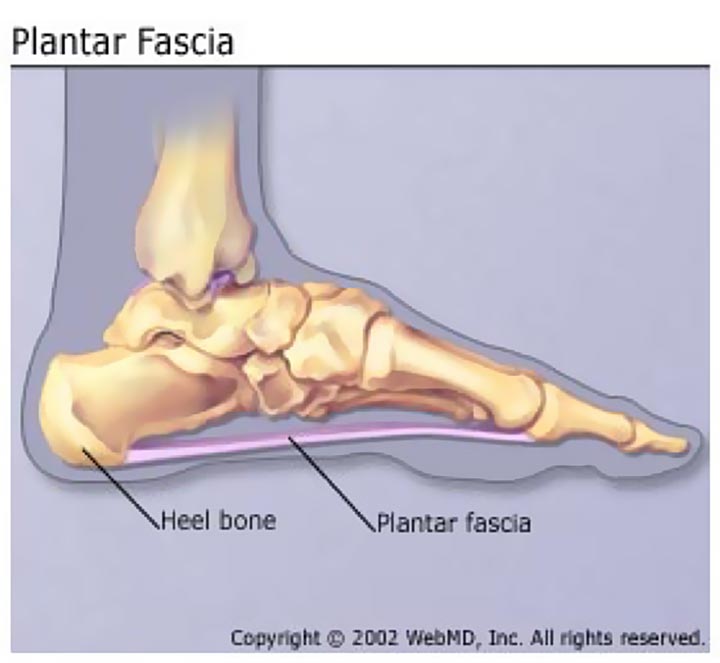
Plantar Fasciitis is a thickening of the plantar fascia, a band of tissue running underneath the sole of the foot.
A number of factors can contribute to plantar fasciitis. It can be due to recent damage or injury, or can be as a result of an accumulation of smaller injuries over the year.
What causes Plantar Fasciitis?
- Taking up a new form of exercise or suddenly increase the intensity of your exercise.
- Standing on your feet for several hours each day.
- Medical conditions such as rheumatoid arthritis or lupus.
- Wearing high-heeled shoes, and switching abruptly to flat shoes.
- Wearing shoes that are worn out with weak arch supports and thin soles.
- Having flat feet or an unusually high arch.
- Having legs of uneven lengths or an abnormal walk or foot position.
- Having tight Achilles tendons or ‘heel cords.’
- Being overweight.
What is the treatment for Plantar Fasciitis?
There are several types of treatment available. You should discuss which option are best for you with your practitioner.
- Heel pad: In plantar fasciitis over-the-counter or custom-made orthotics, which fit inside your shoes, may be constructed to address specific imbalances you may have with foot placement or gait.
- Stretching: Stretching exercises performed three to five times a day can help elongate the heel cord.
- Ice: You may be advised to apply ice packs to your heel or to use an ice block to massage the plantar fascia before going to bed each night.
- Pain relievers: Anti-inflammatory drugs such as ibuprofen, are often helpful in decreasing inflammation and pain.
- A night splint: A night splint is sometimes used to hold your foot at a specific angle, which prevents the plantar fascia from shortening during sleep.
- Ultrasound: Ultrasound therapy can be performed to decrease inflammation and aid healing.
- Steroid injections: Anti-inflammatory steroid injections directly into the tissue around your heel may be temporarily helpful.
- Walking cast: In cases of long-term plantar fasciitis unresponsive to usual treatments, your practitioner may recommend that you wear a short walking cast for a few weeks. This ensures that your foot is held in a position that allows the plantar fascia to heal in a stretched, rather than shortened, position.
The best rehab for Plantar Fasciitis?
- No running, walking or any other activity which causes pain either during, after or the following day.
- Night splint - wear a plantar fasciitis night splint for as long as is comfortable.
- Maintain fitness - by swimming or cycling and use the opportunity to work on upper body strength.
- Gentle stretching - if pain allows. Stretching the plantar fascia is essential but in addition all the muscles of the lower leg should be stretched - including the calf muscles and the tibialis anterior at the front of the leg. Continue stretching daily throughout the rehabilitation phase and long after the injury has healed.
And naturally we highly recommend deep tissue massage to help release tension in the deep calf muscles that put strain on the plantar fascia, as well as some soft tissue therapy in the deep fascial compartments of the foot and Ultrasound Therapy to help remove the inflammation. All of which are available at our clinic at Shelley Manor Medical Centre.
Contact Amanda to discuss your options on amanda@intulohealth.com or ring 01202 443892 to book your appointment with Amanda or Rachel.


